19 Apr India’s Fight Against Anaemia
This article covers “Daily Current Affairs” and the Topic of India’s Fight Against Anaemia.
SYLLABUS MAPPING:
GS-2-Social issue- India’s Fight Against Anaemia.
FOR PRELIMS
What is Anaemia? What are the key interventions under the Anaemia Mukt Bharat (AMB) initiative?
FOR MAINS
What challenges does India face in combating anaemia, and how can community-based approaches help overcome these challenges?
Why in the News?
India, home to the world’s largest adolescent population, continues to battle high rates of anaemia, a major public health challenge affecting women, children, and adolescents. Recently, anaemia has been in focus due to renewed efforts under the Anaemia Mukt Bharat (AMB) initiative, which aims to tackle the issue through iron-folic acid supplementation, deworming, fortified foods, and behaviour change campaigns. With its integrated, community-based approach linking maternal, child, and adolescent health, AMB is gaining attention as a global model for tackling nutritional anaemia. The government’s emphasis on scaling up this evidence-driven programme reflects its critical role in breaking the cycle of malnutrition and improving national health outcomes.
What is Anaemia?
Anaemia is a medical condition in which the number of red blood cells (RBCs) or the haemoglobin concentration within them is lower than normal. Haemoglobin is a protein in red blood cells responsible for carrying oxygen from the lungs to the rest of the body. When haemoglobin levels drop, the body’s ability to transport oxygen decreases, leading to fatigue and other symptoms.
Key Points:
1. Primary cause: Iron deficiency (Iron Deficiency Anaemia – IDA).
2. Other nutritional causes: Deficiency of folate, vitamin B12, and vitamin A.
3. Non-nutritional causes: Blood loss (e.g., menstruation, ulcers), infections (like malaria), chronic diseases, genetic conditions (like thalassemia), and exposure to toxins (e.g., fluorosis).
Anaemia status in India and globally
| Aspect | Global Status | India Status |
|---|---|---|
| 1. Overall Prevalence | ~500 million women (15–49 yrs) and 269 million children (under 5) affected | Among the highest global burden of anaemia |
| 2. Women Affected (2019) | 30% of non-pregnant and 37% of pregnant women had anaemia | 57% of women (15–49 yrs) anaemic as per NFHS-5 |
| 3. Children Affected (2019) | 269 million children under 5 had anaemia | 67% of children (6–59 months) are anaemic (NFHS-5) |
| 4. Main Cause | Iron Deficiency Anaemia (IDA) most common | Nutritional causes (iron, folate, B12, Vitamin A) + non-nutritional (e.g., malaria) |
| 5. Impact on Health | Cognitive delays, maternal and child mortality, reduced productivity | Similar impacts: impaired development, LBW babies, perinatal complications |
| 6. High-Risk Groups | Women, young children, and pregnant women | Adolescent girls, pregnant/lactating women, and young children |
| 7. Progress and Challenges | Global decline is slow; targets for 2030 were set by the WHO | Prevalence increased despite efforts; requires intensified action |
| 8. Government Response | WHO guidelines and country-specific programs | Anaemia Mukt Bharat (2018) with a 6x6x6 strategy targeting all age groups |
What are its symptoms?
Anaemia manifests with symptoms such as fatigue, diminished physical work capacity, and shortness of breath. It serves as an indicator of poor nutrition and various health issues. Common and non-specific symptoms of anaemia include tiredness, dizziness or feeling light-headed, cold hands and feet, headache and shortness of breath, particularly during exertion.
Reason for more Anaemia in India
Nutritional Causes
1. Iron Deficiency: Most common cause due to low intake of iron-rich foods (like leafy greens, lentils, meats). Iron loss due to menstruation, pregnancy, and parasitic infections worsens the deficiency.
2. Deficiency of Other Micronutrients: Low levels of folate, vitamin B12, and vitamin A also contribute to anaemia. These nutrients help in the production and maintenance of healthy red blood cells.
3. Poor Dietary Diversity: Heavy dependence on cereal-based diets with low bioavailable iron and low consumption of fruits, vegetables, and animal protein.
Non-Nutritional Causes
1. Parasitic Infections & Deworming Gaps: Worm infestations, particularly in children, lead to chronic blood loss and poor iron absorption.
2. Frequent Pregnancies & Early Marriages: Short birth intervals and teenage pregnancies increase iron demand, depleting iron stores in women.
3. Inadequate Maternal Health Services: Limited antenatal care, poor iron-folic acid compliance, and gaps in deworming & supplementation programs.
4. Lack of Awareness & Behavioural Barriers: Myths, taboos, and lack of awareness about iron-rich diets and supplements hinder prevention efforts.
5. Genetic and Chronic Disorders: Diseases like thalassemia, sickle cell anaemia, and chronic kidney disease affect haemoglobin levels.
Govt initiatives and policies to tackle Anaemia
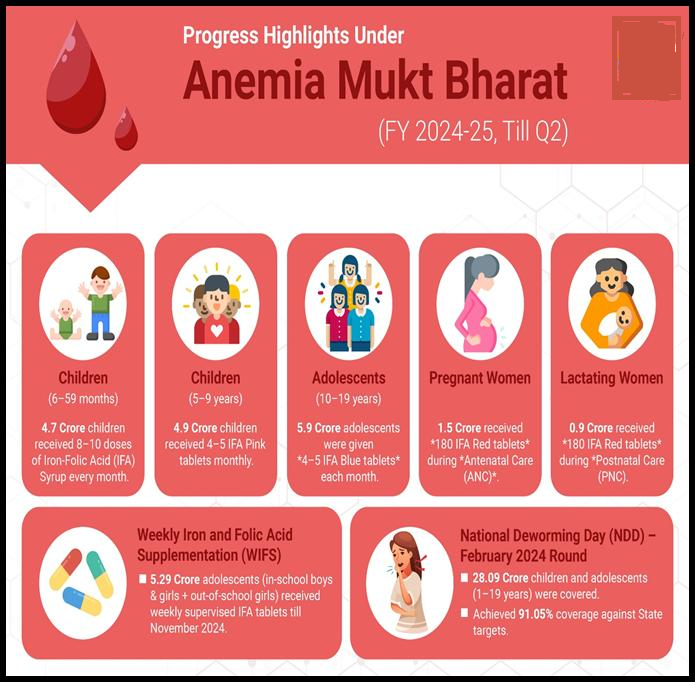
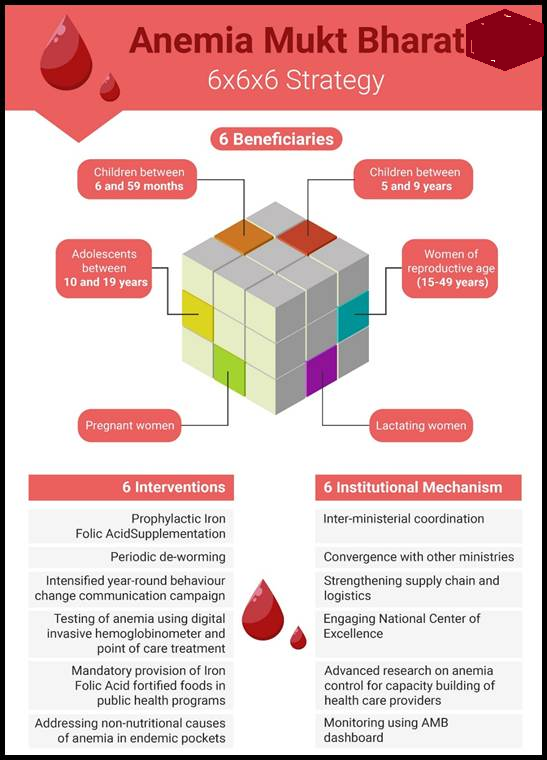
1. Anaemia Mukt Bharat (AMB): Launched in 2018 with a 6x6x6 strategy targeting six age groups through six interventions like IFA supplementation, deworming, fortified food, testing, and awareness.
2. National Iron Plus Initiative (NIPI): Provides Iron and Folic Acid (IFA) supplements across the life cycle—from infants to women of reproductive age—via schools, health centres, and Anganwadi workers.
3. Weekly Iron and Folic Acid Supplementation (WIFS): Focuses on adolescents (10–19 years), especially school-going children, by giving IFA tablets every week and conducting biannual deworming.
4. Poshan Abhiyaan (National Nutrition Mission): Aims to reduce anaemia, stunting, wasting, and undernutrition through convergence between ministries, community engagement, and digital monitoring.
5. Food Fortification Program: Mandatory fortification of staple foods (rice, salt, wheat flour) with iron, folic acid, and vitamin B12 in schemes like Mid-Day Meals, ICDS, and PDS.
6. National Deworming Day (NDD): Observed twice a year (Feb 10 & Aug 10) to reduce worm infestations in children and adolescents (1–19 years), a major cause of iron loss.
7. Comprehensive Antenatal Care (ANC): Pregnant women are provided with daily IFA tablets, deworming, and nutrition counselling as part of their routine health check-ups.
8. Screening for Genetic Disorders: Initiatives to detect and manage thalassemia, sickle cell anaemia, and other inherited blood disorders, especially in tribal and high-risk regions.
9. Behaviour Change Communication (BCC) Campaigns: Nationwide awareness programs (like “Solid Body, Smart Mind”) promote healthy eating, IFA compliance, menstrual hygiene, and delayed early pregnancies.
Challenges in Tackling Anaemia
1. Poor Dietary Diversity: The Majority of the population, especially in rural areas, depends on cereal-based diets that are low in iron and other essential micronutrients. Low consumption of animal-source foods, fruits, and vegetables limits iron absorption.
2. Low Compliance with Iron-Folic Acid (IFA) Supplementation: Irregular intake due to side effects (nausea, constipation), lack of awareness, or non-availability of tablets. Stigmas or myths around IFA tablets in some communities.
3. Inadequate Health Infrastructure: Limited availability of trained health workers, point-of-care diagnostic kits, and regular stock of supplements in remote or tribal areas. Weak follow-up mechanisms.
4. High Prevalence of Worm Infestation: Poor sanitation, lack of deworming awareness, and low toilet coverage lead to intestinal worm infections that cause chronic blood loss.
5. Early Marriage and Frequent Pregnancies: Teenage pregnancies and short birth intervals increase iron demands and reduce women’s nutrient reserves, making them more anaemic.
6. Inadequate Antenatal and Postnatal Care: Many women miss ANC visits or don’t complete the full course of supplements. Poor follow-up for postnatal IFA consumption and nutrition counselling.
7. Limited Awareness and Behavioural Barriers: Lack of knowledge about iron-rich foods, appropriate cooking methods (e.g., using iron utensils), and dietary habits that enhance or inhibit iron absorption.
8. Underreporting and Poor Monitoring: Inadequate real-time data, fragmented health records, and delayed reporting affect timely intervention. Limited use of digital tools in some regions.
9. Non-Nutritional Causes Often Neglected: Conditions like malaria, thalassemia, fluorosis, and chronic diseases that also cause anaemia are not adequately screened or addressed in many programs.
Recommendation
1. Enhance Nutritional Interventions: Promote dietary diversification through awareness programs and kitchen gardens. Encourage consumption of iron-rich and fortified foods, especially in school and Anganwadi meals.
2. Strengthen IFA Supplementation and Deworming: Ensure uninterrupted supply of quality IFA tablets and deworming drugs. Address compliance issues through community-based counselling and follow-up.
3. Invest in Health Infrastructure: Train more frontline workers and ensure last-mile delivery of services in remote areas. Equip health centres with diagnostic kits and point-of-care anaemia testing tools.
4. Improve Antenatal and Adolescent Care: Ensure universal ANC coverage, postnatal care, and early anaemia detection. Expand school health programs for adolescents, especially in rural and tribal areas.
5. Behaviour Change Communication (BCC): Intensify awareness campaigns on nutrition, menstrual hygiene, delayed pregnancy, and iron supplementation. Use local influencers, digital platforms, and community mobilisation for behaviour change.
6. Screening and Management of Genetic Disorders: Conduct routine screening for thalassemia, sickle cell anaemia, and other conditions in high-risk groups. Integrate with state health schemes and ensure follow-up treatment.
7. Data-Driven Monitoring and Accountability: Use real-time data tracking and dashboards for programme effectiveness. Promote inter-ministerial convergence and accountability mechanisms under Poshan Abhiyaan.
Conclusion
Anaemia remains one of India’s most persistent public health challenges, especially among women, children, and adolescents. Despite multiple initiatives, progress has been slow due to a complex interplay of nutritional, socio-economic, and systemic factors. The Anaemia Mukt Bharat initiative represents a promising step towards integrated, life-cycle-based interventions. However, to meet national and global nutrition targets, India must adopt a multi-sectoral, community-driven approach, combining nutrition, health, education, and sanitation reforms. Bridging gaps in infrastructure, awareness, and service delivery is essential to eliminate anaemia and ensure a healthier, more productive population.
Download Plutus IAS Current Affairs (Eng) 19th April 2025
Prelims Questions
Q. Anaemia continues to be a major public health challenge in India, particularly affecting women, children, and adolescents. Discuss the causes, government interventions, and key challenges in addressing anaemia in India. Also, suggest a way forward.
(250 words, 15 marks)
- E-NAM and the Transformation of Agricultural Marketing in India - April 17, 2026
- Indian Railways: Journey from Steam Engines to a Modern Transport Backbone - April 16, 2026
- Mission Poshan 2.0: Strengthening India’s Nutrition Ecosystem - April 15, 2026






No Comments